Hospital Fun
I staggered into Northeast Baptist Hospital on Wednesday, February 25th with complete trepidation. The admissions representative commented, as I was nervously filling out intake paperwork and Mom was parking the car, that she always feels bad for cancer patients. “I could tell you had cancer right away when I looked at you; I saw your papers and said ‘Yep! She’s going to oncology.’” “Uhhh yeah, thanks,” I muttered, not quite sure how to take that. And here I thought I was having a decent aesthetics day….
I was taken to room 130 on the oncology unit (all private suites, thank GOD), asked to change into a gown, and immediately given a pitcher of water and instructions on how to operate the bed and call button. It was all so surreal. I realize that most people reading this have experienced this by now, but I hadn’t and was dumbstruck at the idea of having to go into the hospital on—quite literally--my LAST day of treatment. Such is my effing luck. I was admitted at 11:00 AM and, save a series of blood tests, Mom and I were basically left alone. Given the effect of Tylenol, my vitals were somewhat normal--as good as can be expected for a cancer patient, anyway--and the doctors were thus not that concerned with me: I was more of an observation patient than a critical patient. The Infectious Disease doctor, a wonderful man named Dr. Wood, visited me later in the afternoon. He basically called me a mystery: I had pneumonia but they weren’t sure what kind and, until they could discern if it was viral, fungal, bacterial, or otherwise, they were going to put me on high doses of five different IV antibiotics. A few minutes later, a Respiratory Therapist (RT) came to my room to administer a breathing treatment and then ask me to hock sputum into a cup (very ladylike, I know). To that, I explained that my cough was dry and that nothing was coming up but, as per her instructions, she insisted that I make a valiant effort. I would later learn that the first run proved fruitless based on the lab results: Not enough “juicy” sputum to draw a conclusion. Gag.
That afternoon a gorgeous bouquet of flowers arrived from Rene’ and Randy. Not only did they brighten my room, but everyone who entered my creepy lair commented on how lovely they were. Rene’ said that she insisted on a PINK vase and if they didn’t have a PINK vase, they needed to find one. Indeed, it was bright fuchsia. Given my lack of hair, makeup, and jewelry, I appreciated the touch of femininity, so I send my sincerest thanks to the couple I like to call R-squared. Mom left on Wednesday night just before I was served what my friend and former college roommate, Lissa, has coined “Chicken Fried Meatloaf.” I texted her that I had no idea whether I was eating chicken fried steak or meatloaf (and, let me tell you, I am NOT exaggerating; I don’t have expectations beyond the ability to identify what I’m eating as evidenced by the fact that I actually like airplane food). The mystery meat was completely inedible and it lent full credibility to the old joke that hospital food sucks. It does.
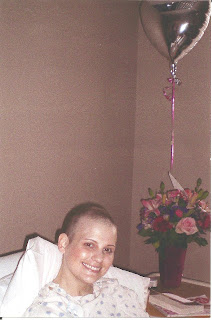 |
| Posing with Rene's flowers |
The pulmonologist referred by Dr. Wilks arrived around 6:30 when I was eating “dinner” (the jury’s still out as to whether or not it was edible). Dr. Deal said that I was looking okay but that a bronchoscopy may be necessary before I leave in order to get a definitive diagnosis. “It’s somewhat invasive, though, so we’ll only do it if you don’t respond to treatment between now and then.” He clarified that, while my temperature may have dissipated, my cough was clearly getting worse.
Later that night, I was awakened no less than four times for my vitals (temperature, blood pressure, pulse oxygenation) and to change out my IV antibiotics. I tallied only a few hours of precious sleep and was exhausted the next morning.
Hospital Day 2: Thursday, February 26, 2009
I still managed to feel pretty good on Thursday—able to shower and brush my teeth in the bathroom without assistance--and an admissions department rep came to my room to give me discharge plans (Do you have someplace to go? Do you have someone staying with you for a few nights?). Even though they didn’t have a specific diagnosis, I was stable and my temperature had remained normal, though my cough was still problematic. All signs were pointing toward going home tomorrow and I couldn’t be happier. Family friends Jackie and Charlie Wright sent a beautiful bouquet of bright red tulips that could almost be mistaken for roses and, along with Rene’s flowers, I couldn’t help but feel loved and supported. My room, at that point, was definitely, unmistakably, a GIRL’S room.
Earlier in the day on Thursday, I was told that the on-call oncologist covering for Dr. Wilks had ordered two units of blood to raise my ridiculously low red cell count. I waited patiently for awhile, then realized that, as the night progressed, the later the blood arrived would directly affect my quality of sleep as clinical staff would have to awake me every few hours to check my stats and change the blood bags. I should clarify that, at this point, I was freaking exhausted. You get very little sleep in a hospital and, combined with a debilitating cough, it’s safe to say that I was getting absolutely none. The blood was ordered at 2:00 pm but wasn’t delivered until close to 8:00 that night. Both transfusions would take four hours each which, after one sleepless night, seemed cruel and agonizing that I’d be awakened at midnight and 4 AM. Additionally, vitals are taken every four hours but they were not on the same schedule as the blood bank, so I knew I’d be awakened at 2:00 and 6:00 AM for those. In the wee hours of the morning, as scheduled, the Certified Nursing Assistant (CNA) wheeled the mobile vitals machine into my room and informed me that I had a fever of 102.0. My pillow and hospital gown were damp with sweat so, on one hand, I wasn’t exactly surprised but, on another, I was shocked since I was on so many IV antibiotics. My coughing fits grew worse and Becky, the CNA, was unfortunate enough to witness one of them. She took my pulse ox on a whim and found that it was 77. Note: A pulse oximeter is a medical device that clamps onto a finger and measures the level of oxygen saturation in blood; blood delivers oxygen to the cells and, with a low pulse ox, organ function declines. I thought that 77 was a passing grade (C’s make degrees, baby), but my nursing team was all aflutter fetching a nasal cannula and hooking me up to O2. “We don’t like it fall below 90,” she explained. Every point beyond that is even more dangerous, so my pulse ox was no bueno. Then again, my incessant coughing and gasping for air wasn’t exactly a sign of thriving health. I felt so much relief from the oxygen that I didn’t mind in the least the irritation of two prongs infiltrating my nostrils.
And yet, I couldn’t sleep that night even after getting O2. Robert, one of the nurses, brought me a book of paintings illustrated by cancer patients depicting their experiences with chemo and radiation. I flipped through it for another two hours (long after home decorating shows on HGTV were replaced with infomercials), and eventually got an estimated three hours of sleep. At some point, a horrific coughing spell during the night necessitated that the nasal cannula be replaced with an actual oxygen mask after they determined that the prongs were not delivering enough precious O2.
Hospital Day 3: Friday, February 27th, 2009
At the inhumane hour of 8:00 AM, I was awakened by a transporter with a wheelchair: “Your doctor ordered chest x-rays. Hop on!” Despite the fact that I was…….ohhhhh, gee, I don’t know….. IN A HOSPITAL BED, they seemed oblivious to the fact that I felt awful: nauseated, exhausted, and chilled. Once in the radiology suite I couldn’t lift myself out of the wheelchair so they managed to take the x-rays with me sitting down--in my wheelchair--in the radiology department--although the “take a deep breath” portion of the show was not gonna happen. I explained to them that I had pneumonia and that doing so was impossible, so they worked with whatever lung capacity remained. To hell with accuracy.
I returned to see my breakfast tray awaiting me and the odor of eggs permeating my room. “Please get this out of my sight,” I said, shooing it away with a wave of my hand, diva-fashion. “Are you nauseous?” The nurse asked. “VERY,” I emphasized wincing with a subconscious gag reflex.
After the x-ray, still early in the morning, I called mom’s cell and demanded to know: “WHERE THE HELL ARE YOU? I NEED TO PEE!! She replied that she was almost here but not close enough for my immediate needs, so I resigned myself to pushing the nurse call button. I summoned Ann and asked her to help me get out of bed as I was now too weak to do so on my own without falling.
“You need a potty chair,” she stated. I stared at her blankly, uncomprehendingly. “What?.....No!....I mean, are you sure? Because, see, I can use a regular toilet with help” I mock-asserted with desperation.
“Nope, we need to put a potty chair by your bed. You’re too weak and we don’t want you falling.” She returned with a white plastic monstrosity: a veritable dignity-sapping piece of equipment that I deigned to use, especially given the fact that I didn’t think this day would come for another 55 years. I was humiliated, but it clarified just how sick I really was.
Not minutes after using the ill-be-spoken potty chair, Mom arrived just in time for Dr. Wood to stop by (and since doctors were taught in med school to wait approximately one-half second between knocking and entry, I was lucky to have escaped an audience for my potty chair debut). He told me that they still didn’t have a conclusive diagnosis (“the sputum wasn’t sufficient”) but that, disturbingly, my potassium level had plummeted. I asked whether or not that would have any correlation with the pneumonia; he shook his head no and said that it was another issue altogether. I’d be getting two bags of potassium between courses of antibiotics. In fact, I was already aware that potassium helps to regulate heart rate and hydration, so I was suddenly paranoid that my heart was now defective. Dr. Wood also mentioned that I may be moved up to the Progressive Care Unit (PCU) for closer observation and more thorough care if I failed to get better in the next day or so. It also happened to be one step away from the dreaded ICU…. I was terrified.
“Mama, if I go to the PCU I’m not coming out of here alive. I just know it,” I said, trying not to cry.
“Baby, I’m not going to let anything happen to you,” she responded with a decidedly stiff upper lip and white-knuckle grip on my bed rails. “But, this is where your attitude comes in. You MUST be POSITIVE. You have to be STRONG through this,” she exclaimed while grabbing my left hand. “You are a fighter. I raised a FIGHTER! And if there’s ever a time you aren’t strong enough to fight for yourself, you know I will fight for you, because that’s what mothers do.” I’ll never forget that strength and resolve in her voice….she very consciously forced me to rally.
Later that day, I learned that Dr. Deal was out of town for the weekend and that he had turned my care over to Dr. Marks. Marks entered my room and told me that, based on the fever and worsening cough, they’d be doing the aforementioned bronchoscopy at around 4:00 that afternoon. This day just keeps getting effing better.
“Delightful!” I exclaimed after he told me that he’d be giving me “sleepy meds” and “forget meds” but that I would essentially be awake and alert the entire time. “Are you as excited as I am?!” I asked him with mock enthusiasm.
 |
| The infamous Six Flags dude |
"I'm ALWAYS ready,” he said (with maybe a little too much enthusiasm?).
Muy Bien, I thought. Preparedness is most definitely a good trait when inserting a tube down someone’s nose or mouth. It is also somewhat sexy….. That last sentiment startled me as I suddenly realized that he was young, good looking, and not wearing a wedding band. I was besotted…..and fuzzy-headed in a cartoon-esque sort of way…..and wearing a cloth gown sans makeup……and, the final touch, wearing my glasses which, against my bald head and propped atop the oxygen mask, makes me look like the dancing old man on the Six Flags commercials or some kind of alien aviator. Yeah…….. I didn’t have a chance. The nurse later explained that I was NPO (no food or drink) all day until after my bronch. At that very moment my appetite was returning so the nurse quickly fetched me a pudding and banana and told me to eat up and THEN go NPO after scarfing it down STAT. I’ve never been so grateful for vanilla Jell-O pudding in my life, particularly midday.
Dr. Wood came by and reinforced that they’re still trying to diagnose my condition. An RT would be arriving again to take another sputum sample (“Try to get a good one this time”) but, for now, I would be at the mercy of the hospital for awhile. “You mean I’m not going to go home tonight or tomorrow?” I asked, helplessly. He nearly laughed and said, “I’d plan on staying through the weekend, if not the entire week.” I felt deflated. I absolutely could NOT spend another night in this place: I was sleep-deprived and depressed and SICK of being poked and prodded. A part of me thought I’d undergo this routine procedure, then recover for an hour and be released home with my mom. Soooooo…..yeah, I guess not.
“Is she going to be okay?” My mom asked with a detectable waiver in her voice. Dr. Wood raised his eyebrows and responded, “I certainly hope so. Let’s just take one day at a time and see what the tests show.” Ouch.
Later that day, the RT attempted to take yet another sputum sample, but part deux was also unsuccessful. Later I will learn that one of the hallmarks of my illness is dry cough with no sputum. Imagine that!
 |
| Sarah as characterized by: No hair or makeup but WITH glasses, oxygen mask, hospital gown, hospital bed and a whole lotta chutzpa. |
At 3:00, a full hour before the procedure, a transporter arrived with a wheelchair. I was taken into an Endoscopy room where I was privy to the preparation process of laying out the instruments, positioning me on the bed, and making sure the larger equipment was set out and operating correctly. In my nervous state, the nurse was annoying me with idle chit-chat and Mom was really effing pissing me off with gentle head strokes--such was my atrocious mood (anyone who knows me well knows that I love it when someone strokes my hair….er, bald head). I told Mom to BACK OFF (Hey Mom: sorry about that by the way) and in doing so managed to simultaneously convey that same message to the uber-verbose nurse. They promptly left me alone to stew in my apprehension.
When the doctor arrived and my Mom was excused to the waiting room I asked him a question that had been bothering me all day: “Dr. Marks, how are you able to do the procedure when any movement whatsoever sets me off into a long, awful coughing spell?” I further explained that simply moving my head an inch in either direction would trigger a fit (which, in turn, would make my pulse ox drop quite drastically), so I was dubious that he could successfully administer the procedure. “Essentially, you’re the kind of patient we do these on. I’m not worried,” he responded. I then heard him tell the nurse, “no, I like to go through the throat, not the nose,” and….without warning, an overwhelming calming and numbing sensation overcame me and I realized that I was being sedated. Wowza, this is some good stuff… Okay……YES….
 |
| Bronchoscope |
I was in Recovery. Mom was at my left side and the nurse was a few feet away. I squinted to see Dr. Marks charting at the nearby counter in front of me, but twisted completely around in his chair as he looked in my direction with furrowed brow and obvious concern as I coughed uncontrollably on the gurney. I learned later that it was well after 6:00 PM and I was still coming out of my drug-induced stupor, despite being out of Endo for over an hour.
“They said you did really well,” Mom said.
“What does that mean?” I sputtered.
“You didn’t fight him and they were able to collect a sample. They didn’t get to do a biopsy because you were coughing too much—they were afraid you’d start bleeding--but that’s okay! They got what they needed.”
At 6:30 I was finally able to return to room 130 where my dinner was awaiting me. I ate a few bites, then pushed it away and fell back to sleep, frequently waking myself with mumbles and groans. I had no idea what was on my tray that night, and still don’t know; It was clearly undesired (and most likely undesirable). Whenever I did let out a loud, random “mfffffnnnnn,” I would inadvertently open my eyes to glimpse Mom staring at me from the recliner as she assessed my physical state, making sure that I wasn’t in pain. I remember repeatedly being so embarrassed that I’d made such a loud noise and would squeak out an apology but, I could almost swear, she grinned and actually chortled when she realized that I was totally high and having a trippy dream. This nonsensical mumbling resumed all night (make strange noise, awake, apologize, fall sleep….repeat). It is no surprise that I felt less than rested on Saturday. I doubt Mom did either. However, she had firmly decided to spend the night on Friday, opting instead to go home to briefly care for Lola in the evening and again early the next morning but otherwise staying with me at the hospital. She had refused to leave my side and slept in the bedside recliner with her head propped against the edge of the headrest and her feet resting on the foot of my bed, contortionist style. As with the two previous nights, I was awakened frequently for blood draws, breathing treatments administered every four hours, IV changes, and vitals. I kept asking Mom if I could request for a cot for her, but she refused, saying, “This way I can be close to you and see you at all times. I can’t be this close to you in a bed.” Only a mother…
Hospital Day 4: Saturday, February 28, 2009
Mom left at 8:00 AM to walk Lola and, during that time, Dr. Wood made his rounds. He told me that they now know what I have: Acute Atypical Pneumocystis—typically found in patients with full-blown AIDS (yes, I was tested and no, I don’t have it thankyouverymuch), and that he would be discontinuing certain antibiotics and resuming others. “This is really good news,” he said. “We’re on the right track.” Yet, after two full bags of potassium my level was not yet adequate, so I would be getting a third bag. Subtle Rene’ said that, for encouragement, she tried to track down a stripper in a banana costume. She ultimately couldn’t arrange it because, apparently, bananas aren’t sexy. Thanks for your efforts, R: I’m sure my blood pressure would have also drastically improved.
My pulmonologist’s on-call partner was also on-call that day, and thus their THIRD partner arrived and carefully examined my lungs. “You had a really difficult bronch,” he said, then explained that I had apparently coughed the entire time and Dr. Marks had asked him to keep a close eye on me. “You almost had to go on a ventilator,” he remarked. Later, Mom explained (assuming I was in a better state to accept this) that, while I DID cough incessantly, thus preventing him from collecting a tissue sample, I was a very obedient patient. That is no surprise: I aim to please. I have absolutely no recollection of the procedure but I was apparently awake, alert, and able to converse. So bizarre! The “forget meds” are called a truth serum in that the part of the brain that conceives of lies is temporarily disengaged. Shut down. Closed for business. The patient can only tell the truth and, knowing this, I wondered if I had professed my sudden, temporary infatuation for the doctor. I’m not ashamed. Let the truth be known; I wanted to sexually molest him. I also find it amusing that, along with the anesthesiologist and surgeon who did my mediport surgery, as well as Dr. Wilks during my bone marrow aspiration, the assisting nurse for the bronch told my Mom that I kept rousing during the procedure and she had to give me more and more sedation. “If I had that much they’d have to resuscitate me!” she said. Once again I stipulate: I am not a cheap date.
Hospital Day 5: Sunday, March 1, 2009
As planned, Mom left early on Sunday to take care of Lola. When she returned to my room she informed me of something AWESOME: She saw perverted Elvis (newcomers please see previous posts regarding Elvis’s “personal stimulation” in the infusion room at my doctor’s office). Elvis is apparently a problem child—not only to Cancer Care Centers of South Texas but to NE Baptist Oncology as well. While he was hooked to an IV and loitering in the hallways, Mom once witnessed a nurse shaking an index finger at him and exclaiming with intense exasperation, “GET BACK IN YOUR ROOM!”
Later that day, my nurse came in to change my IV. “Is Elvis here?” Mom asked. “What?” she asked, startled and apparently caught off-guard. I intervened: “I’m a patient at the cancer treatment center across the freeway. Is there someone named Elvis here?” With a heavy sigh, she nodded, rolling her eyes. We laughed, remembering that Elvis gave us quite the show during chemo. Apparently, our rebellious friend had become a public disturbance. “He’s here all the time,” the nurse said, dismayed.
Mom returned to my apartment to collect Lola and Lola Accessories in preparation for transport. Family friends decided that the best way they could help us would be to make the three-hour drive from Rockport to San Antonio and take Lola so that Mom could stay with me at the hospital without worrying. I was still incredibly sick that nothing mattered to me at that time, yet Mom was so grateful that she cried when Susan offered to take my beloved Little Lola off her hands. Much later that afternoon, x-ray came to my room (I was no longer deemed fit for intra-hospital travel) and everyone cleared out as my lungs posed for their glamour shots. That night, since Lola was sent off in her doggie seatbelt, food and toys in tow, Mom was able to relax in the hospital recliner to watch Desperate Housewives. A heartfelt thank-you to Susan and Sandal for their enormous generosity.
I felt terrible that night and, minutes after Mom and I turned off the TV to go to sleep, I heard a whirrrrrrr outside. Shortly thereafter, the room suddenly became unusually warm and I realized that the hospital lost power but that the generator had kicked in. Luckily, the medical equipment (oxygen, IV monitor, pulse ox, etc.) was connected to said generator. Mom looked out the window and noticed that the entire opposite hospital wing, block, and freeway lights were completely dark. Within a short time the room became stuffy and my difficulty with breathing was exacerbated. I complained that my nose was so stuffed up that I had to breathe through my mouth in this thick heat but, with the humidity, even that was challenging: Once again, I felt like I was breathing through a straw. “I can bring you a fan,” the CNA suggested brightly. I, in my horrid mood, said, “That’s just going to make it WORSE! I’m already congested and the dry air will only aggravate it” (I stopped just short of adding, “duh.”) I insisted that she call in a decongestant and, since the on-call oncologist with a less-than-stellar bedside manner was expected to answer the phone, the poor CNA delayed for an hour. I begged her in the wee hours of the morning and she finally acquiesced--because I was, well, a bitch. The doctor prescribed Benadryl and Tessalon cough pearls, which directly affect the lungs and not the central nervous system as does Codeine (I’m highly allergic to codeine and will vomit profusely if ingested). With the aid of medication and an oxygen mask (in use at all times except when I was eating, during they would replace the mask with a nasal cannula), I finally experienced a few precious hours of relief before being awakened for my morning stats.
Hospital Day 6: Monday, March 2, 2009
I woke up on Monday feeling somewhat decent. After determining the cause of my illness, the right antibiotics were identified and, placebo effect or not, I felt confident in my recovery. Dr. Wilks was back in town and made a much-needed appearance (I love that woman!). She told me to “Get used to this place” and “make it your home…..put up some pictures and get comfortable.” In other words, the antibiotics would take effect in time, but that I was here for at least a week. Saddened to hear that, the day was unremarkable and, that night, the nurses offered to move me to a different room with a pull-out bed and more space. We couldn’t resist and were soon transferred to 123. The benefit of the room’s—well--roominess was undeniable but the disadvantage was also clear: Room 130 had overlooked the physician parking lot and I could therefore keep an eye on who came and went, stalker style (and by that point I had started to know who drove what), while room 123 offered a view of a fake garden area and the side of another building. Still, Mama Jackie was able to stretch out at night and I felt less claustrophobic.
Hospital Day 7: Tuesday, March 3, 2009
Dr. Wood arrived on Tuesday morning and told me that I was responding so well to the antibiotics (as evidenced by the convenient, nightly 3:00 AM blood draw results), that he wanted to talk about discharging me on Thursday or Friday. Seeing as I was fully reliant on oxygen, I was somewhat surprised that he thought I was ready. “You’re getting stronger and we’ll send you home with portable oxygen,” he explained, also reiterating that the worst place for a sick person to be—given the risk of hospital-acquired illness—was, in fact, a hospital. I already knew this, given my education and background in healthcare administration (the textbooks called it “iatrogenic illness,” actually), but--oy vey was I leery. Scared, even. My friend Iris visited me with yellow tulips and a gift bag assembled by her toddler son (everything, including the pencil, slinky, eraser, and rubber ball, had a smiley face on it: It was clearly a theme bag. Look out, Lizzie Grubman, PR guru to the stars, you’ve got some competition). As uplifting as it was, I could still accurately be described as down. This was shocking to me. I spent a week lamenting my hospitalization--mentally tabulating the inevitable, extravagant bill I was racking up hour-by-hour, considering all the things I should be doing with my time to find a job, and secretly cursing all those who prevented me from getting more than 4 hours of collective sleep a night. Where was this sudden, surprising depression surfacing from? Although I responded the way one is supposed to when one’s captors announce impending release: “Oh that’s GREAT!,” I was actually very scared. Later that evening, stuffing a portable O2 tank in the back pocket of my wheelchair, Mom took me outside to a courtyard area for some fresh air which made me feel so much better seeing as I hadn’t been outside in six days, and I began to think that perhaps I was ready to go home. Or maybe that was the Ativan talking.
Hospital Day 8: Wednesday, March 4, 2009
On Wednesday I woke up and decided that I didn’t need to use my potty chair anymore. I had had enough humiliation during the last few days in asking Mom to retrieve toilet paper and stand guard as I perched on the makeshift commode only inches from my hospital bed. In complete defiance, I hobbled out of bed without anyone’s help and used the real toilet on my own (but was not allowed to close the bathroom door…hmph). Minutes later, Dr. Marks, my most recent crush, arrived and Mom showed him (as she did the other docs and nurses) a picture of me taken just before my diagnosis: “This is what she really looks like.” He looked at it and said with (if I’m not mistaken) disbelief and incredulity, “This is YOU?” I nodded, and he said, “Well, I recognize that smile. She’s always smiling. Always.” I felt all warm and fuzzy inside. Furthermore, not only did I accomplish the amazing feat of going to the bathroom unattended, but Mom wheeled me outside for almost an hour so that I could breathe fresh air yet again, but this time off the mask and on the nasal cannula for my venture. During that time I managed a long conversation with my friend Theresa which only heightened my spirits as I realized that I was, indeed, physically becoming capable of going home soon. The potty chair remained in my room as a “just in case,” but I didn’t have to use it. When Dr. Wilks arrived that afternoon and said that I would be due to go home on Thursday, I informed her that Dr. Wood indicated Friday as the likely day. “We don’t like to discharge on Friday because, if something goes wrong, you wouldn’t be able to reach me.” At that point, I’d decided that that was totally fine with me…….I’d choose my feather bed and real food over the hospital any day. The best news was that I no longer needed constant O2. For the most part, the nasal cannula (which was a firm downgrade that morning from the mask), lay at my bedside as I learned to breathe normal air unassisted again. Later in the afternoon, I was wheeled down the hall for an echocardiogram just to make sure that the potassium drop wasn’t an indication of heart damage.
On Wednesday I woke up and decided that I didn’t need to use my potty chair anymore. I had had enough humiliation during the last few days in asking Mom to retrieve toilet paper and stand guard as I perched on the makeshift commode only inches from my hospital bed. In complete defiance, I hobbled out of bed without anyone’s help and used the real toilet on my own (but was not allowed to close the bathroom door…hmph). Minutes later, Dr. Marks, my most recent crush, arrived and Mom showed him (as she did the other docs and nurses) a picture of me taken just before my diagnosis: “This is what she really looks like.” He looked at it and said with (if I’m not mistaken) disbelief and incredulity, “This is YOU?” I nodded, and he said, “Well, I recognize that smile. She’s always smiling. Always.” I felt all warm and fuzzy inside. Furthermore, not only did I accomplish the amazing feat of going to the bathroom unattended, but Mom wheeled me outside for almost an hour so that I could breathe fresh air yet again, but this time off the mask and on the nasal cannula for my venture. During that time I managed a long conversation with my friend Theresa which only heightened my spirits as I realized that I was, indeed, physically becoming capable of going home soon. The potty chair remained in my room as a “just in case,” but I didn’t have to use it. When Dr. Wilks arrived that afternoon and said that I would be due to go home on Thursday, I informed her that Dr. Wood indicated Friday as the likely day. “We don’t like to discharge on Friday because, if something goes wrong, you wouldn’t be able to reach me.” At that point, I’d decided that that was totally fine with me…….I’d choose my feather bed and real food over the hospital any day. The best news was that I no longer needed constant O2. For the most part, the nasal cannula (which was a firm downgrade that morning from the mask), lay at my bedside as I learned to breathe normal air unassisted again. Later in the afternoon, I was wheeled down the hall for an echocardiogram just to make sure that the potassium drop wasn’t an indication of heart damage.
Hospital Day 9: Thursday, March 5, 2009--Discharge Day
On Thursday morning, I woke up prepared to go home after having a decent night of sleep with only one coughing spell and no oxygen (the nurses also tend to leave you alone when you’re doing well and about to leave. When snoozing peacefully, the nice ones will forego vitals in favor of saving a limb). Mom took me outside on another long O2-assisted wheelchair venture. The nurse delivered discharge paperwork and informed me that I was only to go home if I agreed to home-based oxygen. Of course I did, and the Praxair representative came to my hospital room to show me how to work the portable oxygen unit, lest I decide to stop breathing on the way home (understandable as they are accustomed to working with COPD and Emphysema patients). I felt confident that I didn’t need constant surveillance, but that was part of the discharge agreement and I was certainly in no position to argue.
I got home at 2:00 and the O2 people arrived around 4:00. They set up the large oxygen machine and showed me how it operates. Eventually that night, I did need the nasal cannula after a coughing fit. I felt mildly ashamed (given my smug attitude insisting that oxygen was soooo passe), but was nevertheless grateful that it was there. I used it sparingly on Friday through Sunday although I did little more than lay in bed, pant, and wonder if my lungs would ever feel normal again. I guess I wasn’t as healed as I thought even though the doctors insisting that my recovery could take as long as two months. Crazy thought that the experts know what they’re doing…..
On Friday I woke up motivated to get better after a much-needed comfortable night of sleep. Mom and I took a short walk and I made sure to manage light activity whenever possible. After some basic stretching and a second light walk, I only needed a small amount of O2. This set the tone for an uneventful weekend.
Yet I was relieved on Monday to still have my oxygen. After the laborious task of showering, my breathing became shallow and I started coughing uncontrollably. I basically spent the day in bed resting as my hardcore oral antibiotics took effect. I ran some light errands with Mom on Tuesday, then took a long nap. I woke up with the desire for a glass of wine (a huge indication of the Return of Sarah and of general health—the early stages, anyway) and found that I FINALLY no longer needed oxygen. The large, imposing plastic box encasing the vital gas became an eyesore in my bedroom, particularly with the extra-long nasal cannula looped on the floor and across my bed. I called Praxair to have them discontinue my O2. “We have to contact your primary care doctor first,” the rep explained. They called back on Wednesday and said that, as per protocol, my doctor required an overnight pulse ox reading sans oxygen assistance before they were permitted to pick it up. If my pulse ox remained steady, as transmitted from the small portable machine to the Praxair office and eventually faxed to my doctor, they would pick it up on Friday. They don’t like to see a pulse ox fall below 90 (and 85 sets off an annoying alarm that I was absolutely, annoyingly used to from the hospital). A man delivered a portable pulse-ox monitor that day and, happily, mine remained steady at 96 that night. On Friday the rep retrieved the machine but told me that the oxygen tanks themselves would likely be picked up next week.
The weekend was dreadfully boring. Mama Jackie struggled through the concept of “doing nothing” as I gladly appointed the couch (and, later in the afternoon, my bed) my haven. We did manage to take another short walk in an effort to exercise my compromised lungs but that was about all the energy that was able to exert that day.
I had a follow-up x-ray for the pneumonia on Monday and they gave me the films to take to my Wednesday oncology appointment. On the way home, I used my professionally trained eye (or not so much) to assess the images. I won’t have confirmation until Wednesday, but I could see small white spots standing out against the gray background of my chest. Is that cancer or scar tissue? They still didn’t know and, most likely, won’t know until we “watch & wait” what my three and six month scans show. No growth = scar tissue; growth = bad news.
Wednesday is my follow-up appointment with Dr. Wilks and then we’re going to Rockport so that Mom can resume her normal life and I can get a change of scenery. I may be doing the same thing there as I would at home (sleep), but at least I can breathe in the saltwater air while doing so. At the clinic I’m so hoping to hear that, despite the spots that remain in my chest, and despite the fact that the radiation oncologist wanted to go through with radiation but now they refuse to screw around with my chest/lungs, I’ll have a somewhat definitive statement of being cancer-free. I may not really know until my first scan in June, but a positive send-off would be much appreciated!
No comments:
Post a Comment